In 2023, the United States recorded 110,037 drug overdose deaths — the highest number in the nation's history. By 2024, that number dropped to 80,391, but opioids still caused more than 54,000 of those deaths (CDC NCHS, 2025). The medical establishment has responded. Both the CDC and the American College of Physicians now recommend non-pharmacological approaches — including chiropractic care — as first-line treatment for pain before considering opioids.
As someone who holds both a Doctor of Chiropractic (DC) degree and a Family Nurse Practitioner (FNP) license, I am trained to prescribe medications — and I am trained to help patients avoid them. This article reviews the 2025 research on chiropractic care vs. opioids for pain management. The data comes from three major studies published in 2025 covering more than 6.8 million patients — the largest body of evidence ever assembled on this question.
TL;DR: A 2025 meta-analysis of over 6.8 million patients found chiropractic care reduces opioid prescriptions by 64% (Pain Reports, 2025). Veterans receiving chiropractic had 90% decreased odds of opioid use. Both the CDC and American College of Physicians now recommend non-pharmacological approaches — including spinal manipulation — as first-line treatment for pain before considering opioids.
How Bad Is the Opioid Crisis in 2025?
The numbers tell the story. In 2023, the United States recorded 110,037 drug overdose deaths, the highest in the nation's history. In 2024, that number dropped significantly to 80,391 — a 26.9% decrease that represents real progress. But opioids still accounted for 54,743 of those deaths, down from 83,140 in 2023 (CDC NCHS, 2025).
The crisis hits rural communities especially hard. CDC data shows that 31.4% of adults in rural areas report chronic pain, compared to 20.5% in urban areas. For communities like Valley, Lanett, and West Point, this is not an abstract statistic — it reflects the daily reality of patients who walk into our clinic looking for relief.
The path from chronic pain to opioid dependence is well documented. A patient visits their doctor with back pain. They receive a prescription for a short-term opioid. The medication masks the pain but does nothing to fix the cause. When the prescription runs out, the pain returns — often worse. The cycle of escalating medication use begins.
This is exactly why the medical community has shifted its approach to pain management. The question is no longer whether we need alternatives to opioids. The question is which alternatives work best and have the strongest evidence behind them.
What Do the CDC and ACP Guidelines Say About Pain Treatment?
Both of the most influential medical guideline bodies in the United States now recommend non-drug approaches as the first step for pain management — not as a last resort.
The CDC's 2022 Clinical Practice Guideline for Prescribing Opioids (CDC MMWR, 2022) states that clinicians should "maximize use of nonpharmacologic and non-opioid pharmacologic therapies as appropriate" and "only consider opioid therapy for acute pain if benefits are anticipated to outweigh risks." This is the nation's top public health agency telling doctors to try everything else first.
The American College of Physicians (ACP) goes even further. Their clinical practice guideline, published in the Annals of Internal Medicine, specifically recommends spinal manipulation as a first-line treatment for acute low back pain — ahead of any medication.
The ACP recommends that "clinicians and patients should select non-pharmacologic treatment with superficial heat, massage, acupuncture, or spinal manipulation" before considering drugs. — American College of Physicians Clinical Practice Guideline, 2017
These are not fringe recommendations from alternative medicine advocates. The CDC and ACP represent mainstream, evidence-based medicine. When both organizations tell physicians to try non-drug approaches first, it reflects an overwhelming body of evidence that the old approach — prescribe painkillers first, ask questions later — was causing more harm than good.
For patients, the practical takeaway is this: if your doctor's first response to your back pain is a prescription, you have every right to ask about non-pharmacological options first. The guidelines support you.
What Does the 2025 Research Show?
The largest-ever meta-analysis on this topic — covering over 6.8 million patients — found chiropractic care reduces opioid prescriptions by 64%. But that is just one of three landmark 2025 studies that collectively represent the strongest evidence ever published on chiropractic care as an alternative to opioids.
The Meta-Analysis (Pain Reports, December 2025)
Published in Pain Reports, this systematic review and meta-analysis combined data from 2 randomized controlled trials and 18 cohort studies covering more than 6.8 million participants. The results were striking: patients who received chiropractic care had 64% lower odds of receiving an opioid prescription (odds ratio: 0.36) compared to those who did not receive chiropractic care.
Even more telling, patients who began chiropractic care early — within 30 days of their initial pain complaint — had 67% lower odds of opioid use. The evidence clearly shows that the sooner patients receive chiropractic care, the less likely they are to need opioid medication.
The Opioid Use Disorder Study (UH Hospitals, October 2025)
Researchers at University Hospitals in Ohio tracked over 49,000 propensity-matched patients to compare opioid use disorder (OUD) rates between those who received chiropractic care and those who used only ibuprofen for back pain. The results: only 0.24% of chiropractic patients developed OUD, compared to 1.51% in the ibuprofen-only group — an 84% relative reduction in addiction risk.
This study is particularly important because it measures addiction, not just prescription rates. It demonstrates that chiropractic care does not merely reduce the number of opioid prescriptions — it dramatically reduces the risk of the most devastating consequence of opioid use.
The Veterans Study (JGIM, 2025)
A study published in the Journal of General Internal Medicine analyzed data from 128,377 veterans receiving care through the VA system. Veterans who received chiropractic care had 90% decreased odds of both early and long-term opioid use compared to those who did not. This is the largest military study on this topic and carries significant weight because VA data is among the most rigorously collected in healthcare.
How Does Chiropractic Compare on Cost and Outcomes?
The evidence for chiropractic care extends beyond opioid reduction. When researchers look at total healthcare costs and patient outcomes, chiropractic-initiated care costs $5,093 per year compared to $9,434 for orthopedic care — 46% less (Chiropractic & Manual Therapies, 2024). Patients who started with a primary care physician fell in between at $5,660 per year.
The cost savings come from reduced reliance on expensive interventions. Research published in Spine found that patients who saw a chiropractor first for low back pain had a 1.5% surgery rate, compared to 42.7% for those who saw a surgeon first. Patients who started with a surgeon were 28 times more likely to end up in surgery.
Patient satisfaction data supports these findings. A 2024 study in the Journal of Patient Experience found that patients were 1.79 times more likely to be satisfied with chiropractic care compared to care from a medical doctor for the same musculoskeletal conditions. And a study published in Spine found that 94% of chiropractic patients with acute radiculopathy achieved greater than 30% pain reduction.
As both a chiropractor and a nurse practitioner, I evaluate each patient from multiple perspectives. If chiropractic care is the best path, that is what I recommend. If a patient's condition requires medical intervention, I have the training to recognize that and refer appropriately. Patients are not choosing blindly — they are getting an honest, comprehensive assessment. Learn more about our integrated care approach.
When Are Opioids Still Appropriate?
Opioids have a role in pain management — but it should be narrow, short-term, and carefully monitored. The goal of this article is not to argue that opioids should never be used. It is to argue that they should not be the default.
Situations where opioid medication may be appropriate include:
- •Post-surgical recovery in the immediate days following a major procedure
- •Cancer-related pain where the underlying disease creates severe, ongoing pain
- •Acute severe trauma such as fractures or crush injuries where short-term pain control is necessary
- •Specific medical conditions where non-pharmacological approaches alone are insufficient
My nurse practitioner training means I know when medication is necessary. I understand pharmacology, drug interactions, and the appropriate use of pain medication in clinical practice. The goal is not to eliminate all pharmaceuticals — it is to avoid defaulting to opioids when safer, equally effective options exist.
When a patient comes to me with back pain, neck pain, or sciatica, I do not start with a prescription pad. I start with an examination, a diagnosis, and a treatment plan that addresses the cause of the pain — through spinal correction and rehabilitative care. For the vast majority of musculoskeletal conditions, this approach produces better outcomes than medication alone — and the 2025 research confirms it. Read about non-surgical back pain treatment options, chiropractic safety research, and how chiropractic compares to other treatment approaches.
Getting Started with Drug-Free Pain Relief in Valley, AL
If you are dealing with low back pain, neck pain, headaches, or sciatica, chiropractic care is a safe, evidence-based first step. The research we covered in this article — spanning more than 6.8 million patients — consistently shows that chiropractic care reduces opioid use, costs less, and produces high patient satisfaction.
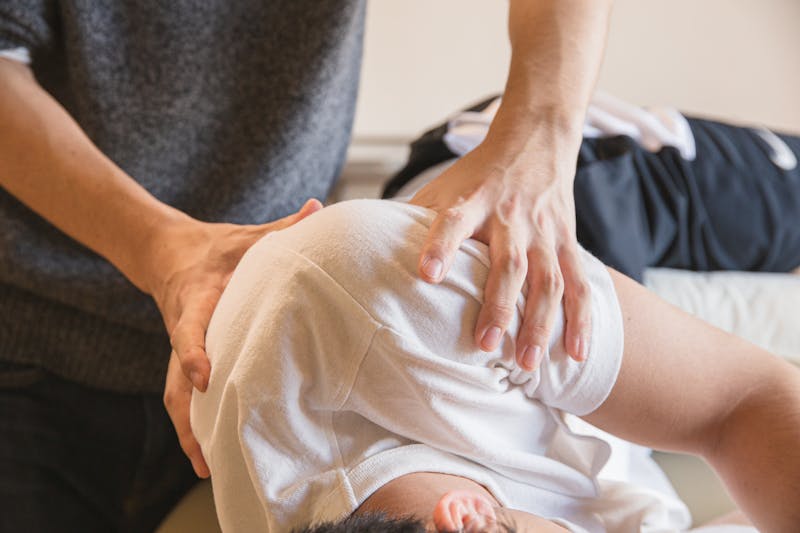
At Chiropractic Unlimited, your first visit includes a comprehensive evaluation to determine if chiropractic care is right for your condition. New patients receive a full examination for just $20. We are located inside Workout Anytime at 3731 20th Ave, Valley, AL 36854, and we serve patients from Valley, Lanett, West Point, LaFayette, and Opelika. Learn what to expect at your first visit and how often you should see a chiropractor for your specific condition.
Dr. Jason Bang's dual DC and FNP credentials mean you are not just seeing a chiropractor — you are seeing a provider who understands both pharmaceutical and non-pharmaceutical approaches and can guide you to the right one. To schedule your appointment, call (334) 203-7032 or book online.
Key Takeaways
- •The evidence is overwhelming: Three 2025 studies covering 6.8M+ patients show chiropractic care reduces opioid use by 64–90%
- •Guidelines support it: Both the CDC and ACP recommend non-pharmacological approaches, including spinal manipulation, as first-line treatment before opioids
- •It costs less and works better: Chiropractic-initiated care costs 46% less than orthopedic care, with a 1.5% surgery rate compared to 42.7%
The evidence is clear: for musculoskeletal pain, chiropractic care should be tried first. If you are ready to explore drug-free pain relief, book a $20 new patient appointment at Chiropractic Unlimited in Valley, AL.
This article is for informational purposes only and does not constitute medical advice. Always consult with your healthcare provider before making changes to your treatment plan. Never stop prescribed medication without guidance from your prescribing provider.



